A Texas-Sized Problem: How to Limit Out-of-Control Surprise Medical Billing
By: Stacey Pogue, Center for Public Policy Priorities
Even diligent patients who ask all of the right questions can get hit with surprise, out-of-network medical bills. This is especially likely to happen in an emergency, when sick or injured Texans must rush to the nearest emergency room and have no ability to choose the doctors who treat them or confirm they are part of their insurance network.
Surprise out-of-network medical bills, sometimes called “balance bills,” happen when insurers and doctors fighting over prices jointly pass the buck to a patient who received out-of-network care unknowingly. The Texas Legislature, long frustrated by this practice, developed a mediation system for surprise bills in 2009 and improved the system in 2015. When patients are able to access the system, it works well. Disputes are almost always resolved with a phone call between the doctor’s office and insurer, with actual mediation rarely needed.
Unfortunately, very few Texas patients have managed to access the system – only 3,824 since 2009. We estimate that 250,000 Texans who have a mediation-eligible health plan will get a surprise, out-of-network medical bill in a two-year period. In other words, only a very small fraction of Texans with surprise bills get help.
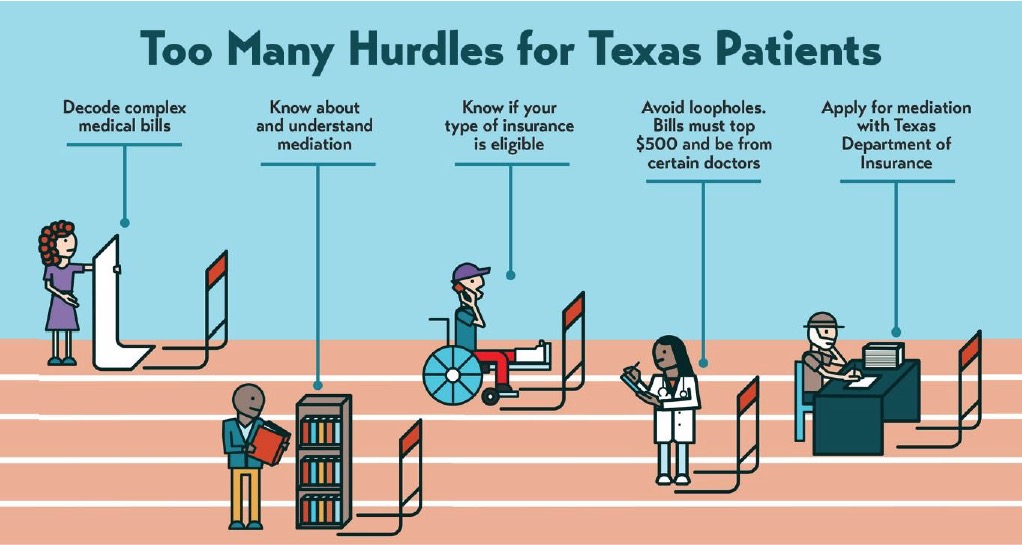
Mediation in Texas is not an automatic consumer protection. Before they can even request mediation, patients must first overcome several hurdles. These include decoding their medical bills, knowing about mediation, and then navigating the mediation system—all while recovering from the illness or injury that sent them to the hospital. Patients who are able to clear these initial hurdles may still be stymied by loopholes that make many surprise bills ineligible for mediation. Patients can only mediate surprise bills from certain doctors, for care provided at certain hospitals, and only if the bill exceeds an arbitrary $500 threshold.
Two recent national studies show that Texas is one of the worst states for surprise medical bills from emergency medical care. CPPP’s analysis of data from Preferred Provider Organization (PPO) plans shows that Texas patients are routinely treated by out-of-network doctors at in-network hospital ERs. A staggering share of hospitals do not have even a single in-network emergency room physician for one or more insurers covering the hospital, guaranteeing that emergency treatment will be performed by out-of-network doctors for many patients. There are more than 300 hospitals in Texas where the hospital itself is in-network, but there is not a single in-network ER doctor available with at least one of the three large insurers examined in this study. On the other end of the spectrum, we found four no-surprise ERs in Texas where the hospital was in-network with all three large insurers in the study and all ER physician billing was also in-network.
In recent years, states including Florida, California, New York, and Illinois have implemented patient-centered policies to address surprise medical bills. They protect patients both from surprise bills and the burdens of navigating a mediation system, while ensuring doctors and insurers can reach a fair price through dispute resolution.
At the end of 2016, both the Texas Senate Business and Commerce Committee and the Texas Department of Insurance recommended expansion of Texas’ mediation system, making prospects good for additional improvements during the 2017 legislative session. There are many ways the Legislature can take incremental, yet meaningful, steps to improve patients’ access to mediation by reducing the barriers outlined in this report. Ultimately, the best and most complete solution for patients that builds off of our existing surprise bill mediation system would incorporate the following principles:
• Protect patients from surprise bills if they did not choose or could not avoid out-of-network care. Especially in emergencies, but also when patients get care at an in-network facility but have no ability to choose an in-network physician, surprise billing should be prohibited. Patients are already responsible for their expected premiums, deductibles, and copayments. They should not be subject to surprise bills beyond those amounts when they unknowingly received care out of network.
• Ensure doctors and other providers and insurers have a trusted system through which they directly settle out-of-network payment disputes. Instead of offloading billing disputes onto patients through surprise bills, insurers and providers should settle their disputes directly using Texas’ mediation system. Providers and/or insurers should initiate mediation, not patients.
• Close the loopholes. All surprise bills stemming from a medical emergency or treatment from an out-of-network provider at an in-network facility should be eligible for mediation with no loopholes. Mediation should cover all providers of emergency care, including facilities like hospitals and free-standing ERs and all physicians practicing at in-network facilities, regardless of their specialty. The arbitrary limit that allows patients to request mediation only for surprise bills that top $500 should be removed, and access should be equal across all public employee plans.





